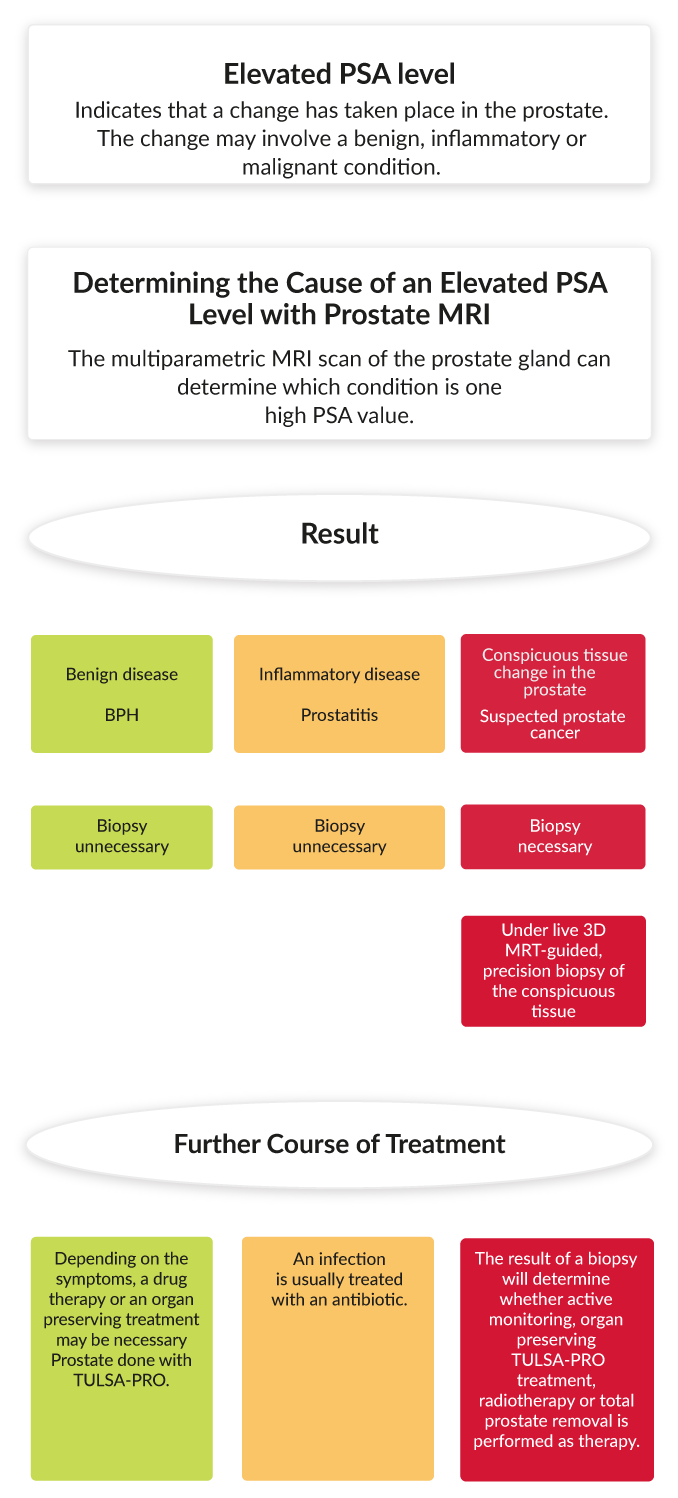
Treatment for Prostate Cancer with MRI-Guided Customized TULSA-PRO
The world’s first minimally invasive TULSA-PRO resection of the prostate was carried out at the ALTA Klinik in March 2017. Since then, the ALTA Klinik has treated about 400 patients with TULSA-PRO. The ALTA Klinik is the only clinic in the world that treats only the diseased area of the prostate – Customized TULSA-PRO
The aim of TULSA-PRO treatment is to destroy prostate cancer while leaving the prostate as functionally intact as possible so as to enable patients to retain normal erectile function and avoid urinary incontinence. Our TULSA-PRO treatment outcomes demonstrate our ability to achieve this aim for our patients.
You are currently viewing a placeholder content from YouTube. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
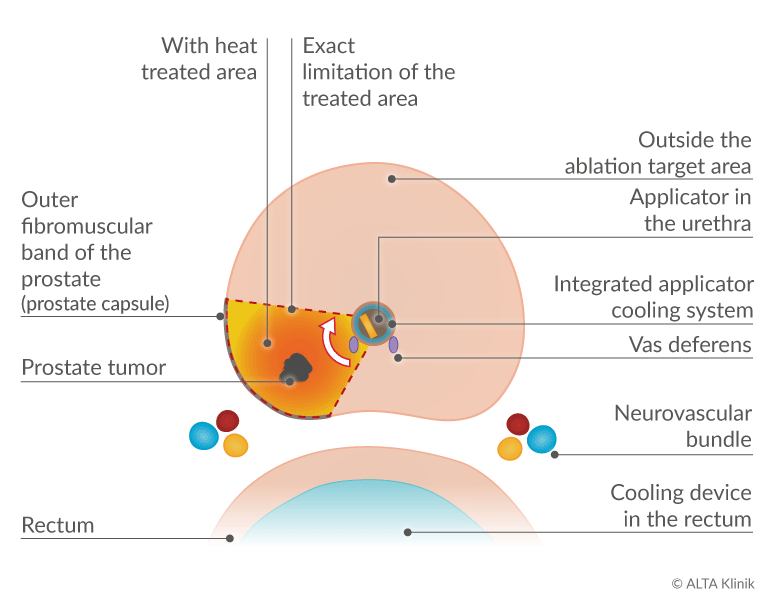
The TULSA-PRO treatment is based on the carefully targeted use of ultrasound energy to destroy, or effectively ablate, diseased tissue in the prostate via thermal coagulation. The ultrasound applicator delivers beams of ultrasound to the tissue in the ablation target area, heating the tissue to the desired range of up to 86 °C. Given that the applicator remains cool throughout the procedure, you doctor can limit the scope of the thermal ablation to precisely demarcated target areas and reduce the risk of damage to healthy prostate tissue and neighboring structures such as the neurovascular bundles, the urinary sphincters and the rectum.
TULSA stands for Transurethral ULtraSound Ablation.
- The term transurethral means “through the urethra.”
- Ablation means the “removal of bodily tissue” (in this case via thermal energy).
- Focal treatment means that the treatment limited to a precisely demarcated target area.
In the case of larger or multiple prostate tumors, the treatment may involve the removal of one-quarter of the prostate (quadrant ablation) or one-half of the prostate (hemiablation). If a patient also suffers from benign prostatic hyperplasia (BPH), the scope of the treatment can be extended to include the excessive tissue growth so as to eliminate the symptoms associated with BPH.
The costs for the TULSA-PRO therapy, including preliminary examinations, are approximately €13,600 for prostate cancer treatment and €14,200 for benign prostatic hyperplasia (tax-free services). These prices may vary depending on individual cases and specific treatment requirements. For precise and up-to-date pricing information tailored to your situation, it is advisable to consult the ALTA Klinik directly.
Quadrant Ablation of the Prostate
The Advantages of TULSA-PRO
The focal application of MRT-guided TULSA-PRO can offer men the following important advantages due to the location of the Prostatecancer:
- Retention of the prostate as an organ
- Retention of erectile function
- Avoidance of urinary incontinence
- Retention of ejaculatory function
- Protection of neighboring structures
Aspects of TULSA-PRO Treatment
Focal TULSA-PRO treatment is based on the targeted and controlled application of ultrasound energy to destroy, or effectively ablate, cancerous tissue via thermal coagulation while at the same time conserving the prostate as an organ. This requires a precise 3D mapping of the prostate tumor using MRI in advance of the procedure, as well as the intraoperative (real-time) control of the ablation procedure via MRI. When mapping the disposition of a tumor, special attention is given to the location of the structures responsible for normal erectile and urinary function, so as to ensure that these remain intact.
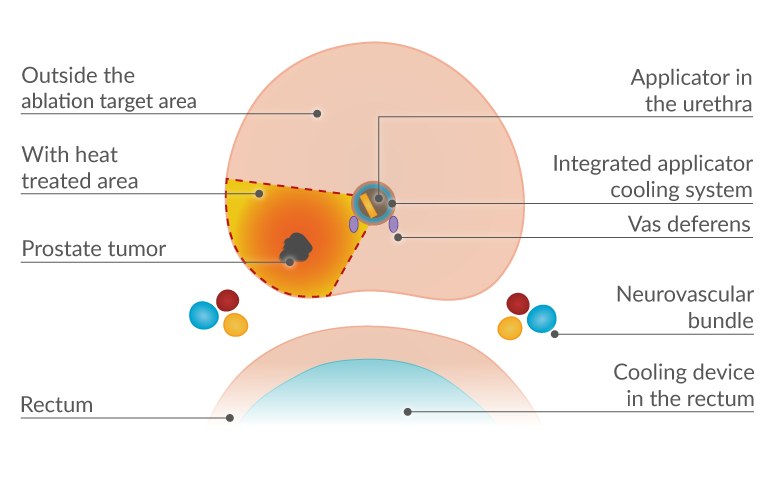
At the start of the minimally invasive procedure, a thin device known as an applicator is inserted through the urethra to the prostate gland, therefore enabling your doctor to remove diseased prostate tissue from within the prostate while preventing damage to other structures in the body such as the rectum and the urinary bladder.
The applicator comes with an integrated cooling system. The cooling system protects the urethra and neighboring structures such as the ejaculatory ducts from excessive heat, particularly when ultrasound energy is being applied to successively ablate the diseased tissue within the prostate.
A cooling device is also inserted into the rectum at the start of the procedure to provide an added measure of safety – in particular, to protect the neurovascular bundles, which run close to the rectum and adjacent to the prostate, and are responsible for normal erectile function.
In addition to precise planning and the exact demarcation of the ablation target area, it is also necessary to precisely control the distribution of thermal energy during the TULSA-PRO procedure. This is accomplished via MR-thermometry, which essentially enables real-time thermal monitoring of the ablation target area and its surroundings, as well as feedback-controlled, ultrasound ablation of the tissue in the ablation target area.
The targeted and controlled application of thermal energy ensures that the diseased tissue, plus an additional safety margin, can be successively and uniformly ablated while tissue outside the target area remains intact.
The diseased tissue that has been destroyed via thermal coagulation is then gradually removed from the body in the course of time. A decline in the patient’s PSA level is also observed.
Mechanism of Action and Aim of TULSA-PRO
The aim of TULSA-PRO is to systematically destroy diseased tissue in the prostate via the application of ultrasound energy. Instead of radiation, the mechanism of action is based on the precisely targeted and controlled delivery of ultrasound beams to heat and effectively ablate the tissue in a circumscribed ablation target area. The desired effect is the destruction of the targeted tissue via coagulation and not vaporization.
With the patient under general anesthesia, the ultrasound energy is applied to the diseased tissue with an applicator that is inserted through the urethra to the prostate. The applicator is a very thin rod-shaped device outfitted with a linear array of 10 independently controllable ultrasound transducers. Turning the applicator to various degrees enables your doctor to reach any area within the prostate.

Applicator with 4 activated transducers
Final planning for the procedure is carried using real-time MRI scans. This means that MRI scans of the prostate and its neighboring structures are generated while the applicator is in position. This allows your doctor to precisely demarcate the ablation target area.
Special attention is also given to the location of the structures straddling the prostate that are essential for normal urinary and erectile function so that these structures can be left intact.
MR-thermometry is used to continuously monitor the intensity and distribution of the ultrasound energy applied to the diseased tissue. The high-resolution scans MRI generated during the procedure enable your doctor to continuously track the temperature at all points in the prostate and its immediate vicinity. This permits intraoperative adjustments whenever necessary and an enhanced degree of patient safety, both with respect to the treatment aim and the prevention of unwanted side effects.
Real-time monitoring of temperature development in an ablation target area in the prostate
The TULSA-PRO Procedure
With the patient under general anesthesia, the applicator is inserted through the urethra to the prostate. The patient is moved into the MRI scanner. A check is made of the applicator’s exact position. Final mapping of the ablation target area is then completed at the MRI console in preparation for the ablation procedure.
The applicator is outfitted with an array of transducers that are each capable of delivering ultrasound energy to raise the temperature of and systematically coagulate the diseased tissue in the precisely demarcated ablation target area in the prostate.
The applicator is also outfitted with an integrated cooling system that cools and protects the wall of the urethra and nearby structures while intense heat is applied to the ablation target area. Additional protection is secured by inserting a second cooling system into the rectum.
MR-thermometry is used to continuously monitor the intensity and distribution of the emitted ultrasound energy in the ablation target area and its surroundings. This enables your doctor to confirm the application of the temperature required to destroy the cancerous tissue.
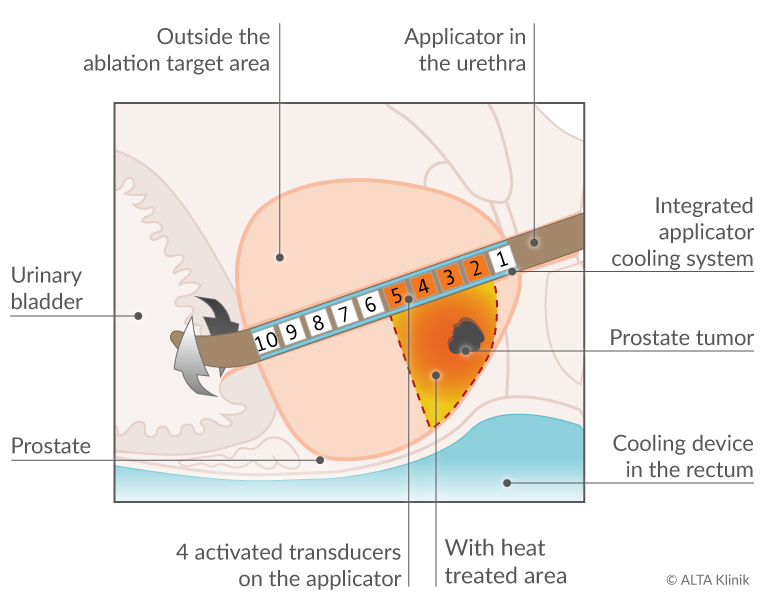
The figure below shows a TULSA-PRO procedure in which transducers 2, 3, 4, and 5 emit ultrasound energy to completely destroy a prostate tumor. Transducers 1, 6, 7, 8, 9 and 10 remain inactive and generate no heat.
TULSA-PRO as a Curative Treatment
TULSA-PRO treatment is performed with curative intent in patients with organ-confined, low and intermediate-risk tumors (Gleason score of 6 or 7).
In addition to a Gleason score within the specified malignancy range, the prerequisites for TULSA-PRO treatment include the availability of precise information about the position, size and extent of a tumor.
Additional prerequisites for focal prostate-cancer treatment include tumor localization, i.e. tumors that are entirely confined within the prostate and have not yet invaded the prostate capsule or spread beyond the prostate (extracapsular extension). Similarly, curative intent presupposes that the cancer has not spread to neighboring structures and that no metastases have formed in lymph nodes, bones or other organs.
Finally, when it comes to retaining normal prostate function, consideration also needs to be given to the spatial relationship between the tumor and the structures responsible for normal prostate function.
TULSA-PRO as Palliative Treatment
TULSA-PRO treatment also represents an effective a form of palliative care:
- For cases of local recurrence
- For cases of high-risk prostate cancer (Gleason score of 8 to 10)
- For cases of non-localized tumors in need of local intervention
Local recurrence
Prostate cancer sometimes reappears after primary intervention involving radiation therapy, IRE, cryotherapy, HIFU and subtotal prostatectomy. In such cases, renewed local intervention often remains a viable option. Such intervention is commonly referred to as salvage therapy. However, both salvage surgery and salvage radiation therapy are often associated with complications.
TULSA-PRO is also an effective form of salvage therapy, for instance, to treat cases of local recurrence after subtotal prostatectomy, radiation therapy, and various forms of minimally-invasive treatment.
TULSA-PRO is an MRI-guided treatment method. In addition to a high degree of precision, this enables the continuous monitoring and control of temperature development in and around the ablation target area (thermometry) and leads to a high degree of safety. TULSA-PRO enables your doctor to precisely target and comprehensively destroy recurrent cancer while at the same time preventing unwanted side effects.
High-risk prostate cancer
Depending on the specific medical indication, TULSA-PRO is also an appropriate form of treatment for cases of high-risk prostate cancer.
Non-localized tumors in need of local intervention
Once prostate cancer has spread beyond the boundaries of the prostate (extracapsular extension) to other structures or organs, it is usually no longer possible to eliminate it entirely. The goal of localized, palliative intervention is to reduce the volume of the tumor (debulking) as much as possible to prevent further growth and avoid complications such as bleeding, urinary retention and urinary incontinence.
Owing to the precision of preliminary MRI planning and real-time intraoperative MRI monitoring, as well as the minimally invasive nature of transurethral ultrasound ablation, TULSA-PRO represents a suitable means of reducing the extent and impact of prostate cancer.
MRI as the Basis for TULSA-PRO
1. MRI scan
Multiparametric prostate MRI is the basis for the initial diagnosis of prostate cancer, as well as for planning appropriate intervention. MRI enables your doctor to ascertain the exact position and spatial extent of prostate tumors. It also provides detailed information about the prostate and its surroundings, information that is necessary for planning and performing focal TULSA-PRO treatment. At the ALTA Klinik, we use a special method of carrying out multiparametric MRI scans of the prostate that we have developed and optimized on the basis of many years of experience.
2. Biopsy
If an MRI scan turns up one or more areas of interest, a biopsy is necessary to rule out or confirm the presence of prostate cancer and assess its degree of malignancy.
Our special MRI-guided prostate biopsy enables us to remove tissue samples from suspicious-looking locations in the prostate with pinpoint accuracy. In keeping with the latest guidelines for prostate biopsy in Germany, we also remove tissue samples systematically from various parts of the prostate. This of the targeted and systematic removal of tissue samples enables better detection rates than other methods alone. Moreover, with the administration of no more than local anesthesia, the procedure is painless.
Given that our biopsy proceeds under real-time MRI control – as opposed to ultrasound-guided – there is no need to insert a probe into the rectum. The removal of tissue samples proceeds neither through the rectum nor the peritoneum, but via a location near the top of the intergluteal cleft. That is why the prophylactic administration of an antibiotic is unnecessary. Once the procedure is complete, the removed tissue samples are carefully examined by our renowned pathologist.
3. Treatment
If the prerequisites are met, we recommend organ-sparing, focal TULSA-PRO treatment.
TULSA-PRO Using Outside MRI Scans
The TULSA-PRO treatment can also be carried out using the results of an outside MRI scan of the prostate, so long as the scans meet the criteria for planning the TULSA-PRO procedure. In order to make this determination, we require a CD copy of the scans along with the radiology report. If a biopsy has already been performed, we will also need a copy of the pathology report.
Our prostate therapy preserves organs and functions! We will be happy to advise you personally:
0521 260 555 44 Arrange a callback Get free advice by telephone now
Get free advice by telephone now
 English
English
 Deutsch
Deutsch  Nederlands
Nederlands